





Navigating the Labyrinth of Ventilator Care: A Lifeline in Jeopardy
The Initial Shock: A Diagnosis and a Desperate Search for Care
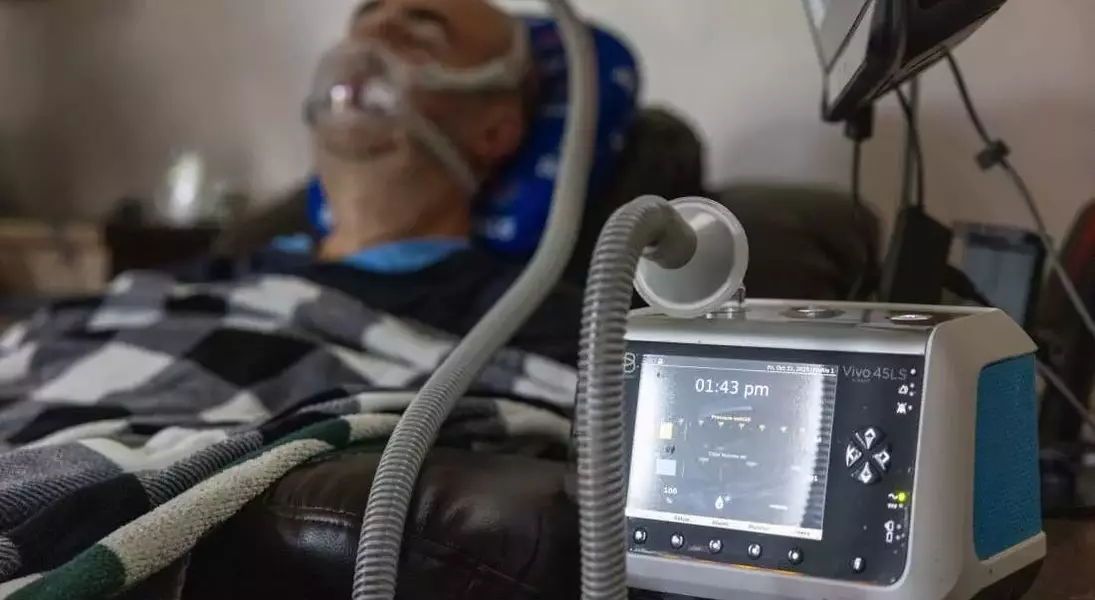
After a series of alarming incidents during a vacation in Mexico, Michael DiPlacido received a life-altering diagnosis of amyotrophic lateral sclerosis (ALS). This progressive neurological condition rapidly led to his reliance on a ventilator, necessitating a tracheostomy. His son, Adam DiPlacido, embarked on a daunting search for a long-term care facility in Missouri capable of providing the specialized support his father required. To his dismay, despite the presence of nearly 500 nursing homes in the state, none possessed the necessary resources or expertise to admit a patient dependent on a ventilator, revealing a critical void in specialized care options.
Systemic Failures: Insurers, Nursing Homes, and the High Cost of Survival
An extensive examination by KFF Health News brought to light widespread deficiencies in the provision of care for individuals unable to breathe independently. Thousands of Americans afflicted by conditions such as spinal cord injuries, strokes, chronic obstructive pulmonary disease, and various neurological disorders find themselves permanently tethered to ventilators. This investigation revealed a disjointed healthcare landscape where patients frequently struggle to obtain appropriate home ventilators from their insurance providers. Families are often compelled to expend vast sums on private nursing care, while those requiring institutionalized care may be forced to relocate to distant states, severing crucial family connections.
Doctor's Dilemma: Battles Over Advanced Ventilators
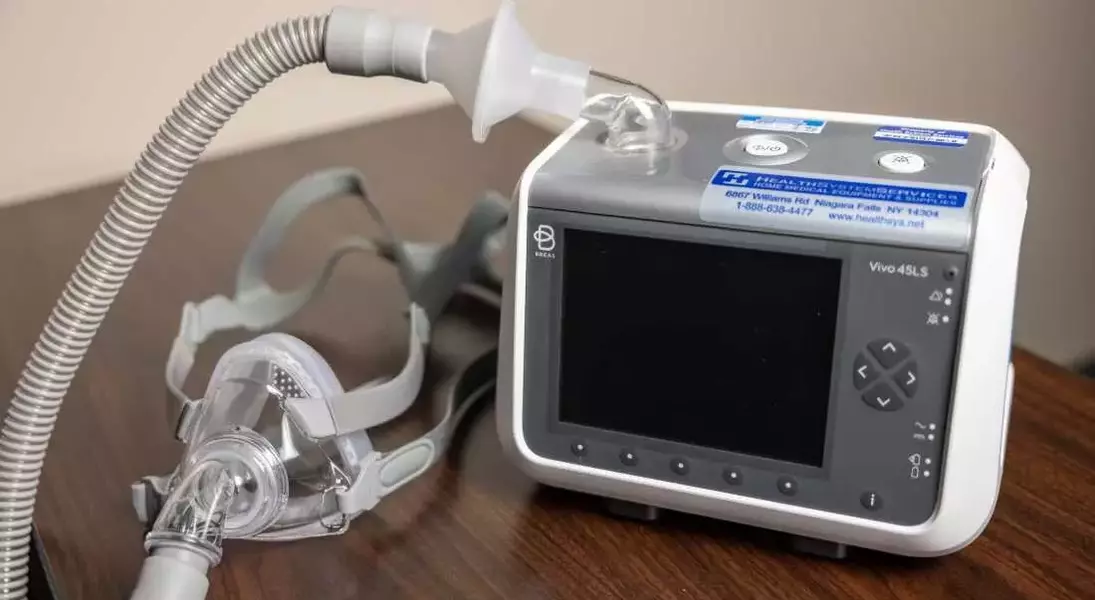
Dr. Tyler Rehbein, an assistant professor of neurology at the University of Rochester who specializes in treating ALS patients, expressed profound frustration with insurance company policies. He noted that insurers frequently expect patients to endure less effective, simpler devices before approving more advanced, battery-powered ventilators, which can cost upwards of $10,000. These advanced units are equipped with vital safety features, such as alarms for collapsed lungs and airway leaks, which significantly enhance patient safety and quality of life. Dr. Rehbein criticized the prevailing mindset of insurers, suggesting they anticipate patients will remain perpetually tethered to wall outlets, rather than investing in portable, life-improving technology.
A Family's Ordeal: Financial Ruin and the Search for Round-the-Clock Support
David Goldstein's journey with ALS began with a subtle limp and rapidly progressed to complete paralysis, rendering him dependent on a ventilator. His ex-wife, Janis Goldstein, who holds power of attorney, described the immense financial and logistical burden of ensuring his constant care. Despite being on a Medicaid waiting list for over a year, the authorized 12 hours of home care daily proved insufficient, forcing them to cover the remaining hours with privately hired nurses. This led to a half-million-dollar expenditure, pushing the family to the brink of financial exhaustion and highlighting the severe inadequacies in state-funded home health programs.
Ventilator Deserts: The Scarcity of Specialized Care Facilities
Adam DiPlacido's desperate search for a nursing home in Missouri capable of caring for his ventilator-dependent father underscored the acute shortage of such facilities. The only potential option informed him they could not accept new patients due to a lack of a respiratory therapist. This forced Michael to seek care outside of Missouri, relocating to a nursing home near Chicago, a five-hour drive from his family. After a brief, unsatisfactory stay, and a stint in a long-term acute care hospital with significant out-of-pocket expenses, Michael eventually returned home with private nursing care, a solution that proved unsustainable until his eventual passing in hospice care.
Addressing the Gaps: Inadequate Reimbursement and Training Deficiencies
Gene Gantt, a respiratory care consultant, pointed out that many state Medicaid programs provide insufficient reimbursement for ventilator patients, failing to incentivize nursing homes to offer high-quality care or invest in weaning programs. He observed that nursing homes often admit patients with tracheostomy tubes even when their staff lacks proper training or when respiratory therapists are absent. David Gifford of the American Health Care Association explained that establishing and maintaining ventilator units is costly, and the limited patient population in non-urban areas often makes such investments financially unfeasible for many facilities.
Insurance Impasses: The 'Fail First' Policy and Repeated Denials
Derek McManus, diagnosed with ALS, faced repeated denials from his insurer for an advanced home ventilator. Despite his deteriorating lung function, the insurer mandated that he first "fail" on a simpler, less effective respiratory assist device, a common practice physicians refer to as a "fail first" policy. His wife, Lesley McManus, expressed profound fear for his safety, given the basic device's lack of critical safety alarms. An independent medical review ultimately overturned the insurer's decision, recognizing the advanced ventilator's necessity for patient safety and quality of life. This case exemplifies the arduous battle many patients face to receive medically appropriate equipment.
A Glimmer of Hope: Innovative Models and Systemic Challenges
The Leonard Florence Center for Living in Chelsea, Massachusetts, stands as a beacon of innovative care, offering an alternative to traditional nursing home environments for ventilator-dependent individuals. Following the Green House philosophy, the center provides small, community-based residences with private bedrooms and common spaces, allowing residents greater autonomy. Utilizing advanced technology, such as mouth- or eye-operated computer tablets, residents can control their environment and maintain a degree of independence. While largely funded by Medicaid and Medicare, the center's reliance on a nonprofit endowment and the absence of similar models nationwide highlight the difficulties in replicating such comprehensive care solutions across the country, especially in the face of potential Medicaid cuts.
